OPP/OMT, Biomechanics
Osteopathic Manipulative Treatment for Chronic Pain: Patient Reservations in Underserved Community
Friday, March 31, 2023
12:00 PM East Coast USA Time

Christine Lomiguen, MD (she/her/hers)
Resident Physician
Millcreek Community Hospital
Erie, Pennsylvania, United States
Presenting Author(s)
Background and Hypothesis: Recent reports reveal greater than 50 million adults (20.5%) in the United States experience pain on most days or every day; however, studies have highlighted general lack of knowledge of osteopathic medicine in underserved communities and need for greater education and outreach. This study investigated knowledge of osteopathic medicine, awareness of its benefits in chronic pain, and willingness to add osteopathic manipulative treatment (OMT) to the care plan after an educational intervention in patients suffering from chronic pain in an underserved community.
After patient education on osteopathic medicine and OMT, investigators hypothesized patients suffering from chronic pain would be more likely to add OMT to their care plan.
Methods: A cross-sectional study was designed in which a survey was administered by convenience sampling to patients with chronic pain at a primary care medical center within an underserved community in Erie, Pennsylvania, USA. This pilot study recruited 26 subjects. All subjects voluntarily participated in educational intervention focused on osteopathic medicine. Study outcomes measured likelihood of patients with chronic pain to add OMT to their treatment plan, before and after education intervention, in relation to location of pain, length of pain, self-reported average pain rating, knowledge of OMT, and awareness of OMT applications in chronic pain. Secondary outcomes included patient reported reservations to addition of OMT to their care plan.
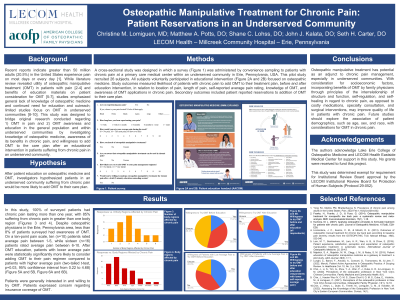
Results: In this study, 100% of surveyed patients had chronic pain lasting more than one year, with 85% suffering from chronic pain in greater than one body region. Despite osteopathic physicians in the Erie, Pennsylvania area, less than 8% of patients surveyed had awareness of OMT. On a ten point pain scale, ten (n=10) patients rated average pain between 1-5, while sixteen (n=16) patients rated average pain between 6-10. After OMT education, patients with lower average pain were statistically significantly more likely to consider adding OMT to their pain regimen compared to patients with higher average pain (two-tailed t-test, p=0.03, 95% confidence interval from 0.22 to 4.68).
Patients were generally interested in and willing to try OMT. Patients expressed concern regarding insurance coverage of OMT.
Conclusion: Osteopathic manipulative treatment has potential as an adjunct to chronic pain management, especially in underserved communities. With consideration for socioeconomic factors, incorporating benefits of OMT by family physicians through principles of the interrelationship of structure and function, self-regulation, and self-healing in regard to chronic pain as opposed to costly medications, specialty consultation, and surgical interventions may have improve quality of life in patients with chronic pain. Future studies should explore the association of patient demographics, such as age, sex, and race, with considerations for OMT in chronic pain.
Acknowledgement of Research Study Sponsors and IRB: The authors acknowledge Lake Erie College of Osteopathic Medicine and LECOM Health Eastside Medical Center for support in this study. No grants were received to fund this project.
This study was determined exempt for requirement for Institutional Review Board approval by the LECOM Institutional Review Board for Protection of Human Subjects (Protocol 29-052).
After patient education on osteopathic medicine and OMT, investigators hypothesized patients suffering from chronic pain would be more likely to add OMT to their care plan.
Methods: A cross-sectional study was designed in which a survey was administered by convenience sampling to patients with chronic pain at a primary care medical center within an underserved community in Erie, Pennsylvania, USA. This pilot study recruited 26 subjects. All subjects voluntarily participated in educational intervention focused on osteopathic medicine. Study outcomes measured likelihood of patients with chronic pain to add OMT to their treatment plan, before and after education intervention, in relation to location of pain, length of pain, self-reported average pain rating, knowledge of OMT, and awareness of OMT applications in chronic pain. Secondary outcomes included patient reported reservations to addition of OMT to their care plan.
Results: In this study, 100% of surveyed patients had chronic pain lasting more than one year, with 85% suffering from chronic pain in greater than one body region. Despite osteopathic physicians in the Erie, Pennsylvania area, less than 8% of patients surveyed had awareness of OMT. On a ten point pain scale, ten (n=10) patients rated average pain between 1-5, while sixteen (n=16) patients rated average pain between 6-10. After OMT education, patients with lower average pain were statistically significantly more likely to consider adding OMT to their pain regimen compared to patients with higher average pain (two-tailed t-test, p=0.03, 95% confidence interval from 0.22 to 4.68).
Patients were generally interested in and willing to try OMT. Patients expressed concern regarding insurance coverage of OMT.
Conclusion: Osteopathic manipulative treatment has potential as an adjunct to chronic pain management, especially in underserved communities. With consideration for socioeconomic factors, incorporating benefits of OMT by family physicians through principles of the interrelationship of structure and function, self-regulation, and self-healing in regard to chronic pain as opposed to costly medications, specialty consultation, and surgical interventions may have improve quality of life in patients with chronic pain. Future studies should explore the association of patient demographics, such as age, sex, and race, with considerations for OMT in chronic pain.
Acknowledgement of Research Study Sponsors and IRB: The authors acknowledge Lake Erie College of Osteopathic Medicine and LECOM Health Eastside Medical Center for support in this study. No grants were received to fund this project.
This study was determined exempt for requirement for Institutional Review Board approval by the LECOM Institutional Review Board for Protection of Human Subjects (Protocol 29-052).
