Medical Education
Disseminated blastomycosis with multi-organ involvement in an immunocompetent host: a case report
Friday, March 31, 2023
12:00 PM East Coast USA Time

Jordan Phelps, DO (he/him/his)
Community Health Network
Indianapolis, Indiana, United States
Presenting Author(s)
Introduction: In a midwestern city known historically for a prior blastomycosis outbreak, this case report demonstrates how B. dermatitidis infection with multi-organ involvement can be easily misdiagnosed and inadequately treated. This case reminds the Osteopathic physician to consider all facets of a patient and their illness not in isolation, but as a whole.
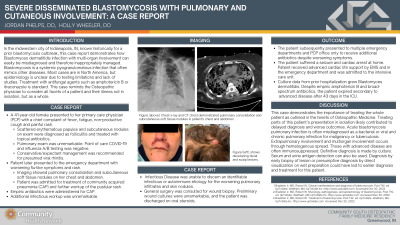
Case Study: A 41-year-old female presented to her primary care physician (PCP) with a chief complaint of fever, fatigue, non-productive cough and painful rash. Scattered erythematous papules and subcutaneous nodules on exam were diagnosed as folliculitis and treated with topical antibiotics. Considering a normal pulmonary exam and negative COVID-19 and influenza point of care testing, conservative management was recommended for presumed viral rhinitis. She later presented to the emergency department with progressive flu-like symptoms and rash. Imaging showed pulmonary consolidation and subcutaneous soft tissue nodules on her chest and abdomen. She was admitted for treatment of community acquired pneumonia (CAP) and further workup of pustular rash. Empiric antibiotics were administered for CAP while further workup was obtained, which proved unremarkable. Infectious disease was unable to discern an identifiable infectious or autoimmune etiology for her worsening skin nodules. Preliminary wound cultures were unremarkable, and the patient was discharged on oral steroids. The patient subsequently presented to multiple emergency departments and her PCP, receiving additional antibiotics despite worsening symptoms. The patient suffered a seizure and cardiac arrest and was admitted to the intensive care unit. Culture data from prior hospitalization grew Blastomyces dermatitidis. Despite empiric amphotericin B and broad-spectrum antibiotics, the patient expired secondary to her advanced disease after 43 days in the ICU.
Discussion: This case demonstrates the importance of treating the whole patient as outlined in the tenets of Osteopathic Medicine. Treating parts of this patient’s presentation in isolation likely contributed to delayed diagnosis and worse outcomes. Blastomycosis is a systemic pyogranulomatous infection that often mimics other diseases. Acute pulmonary infection is often misdiagnosed as a bacterial or viral and chronic pulmonary infection for malignancy or tuberculosis. Extrapulmonary involvement and multiorgan involvement is through hematogenous spread. Those with advanced disease are often immunosuppressed. Definitive diagnosis is made by culture. Serum and urine antigen detection can also be used. Treatment with antifungal agents such as amphotericin B or itraconazole is standard. Diagnosis by early biopsy of lesion or presumptive diagnosis by direct visualization on wet preparation could have led to earlier diagnosis and treatment for this patient.
Case Study: A 41-year-old female presented to her primary care physician (PCP) with a chief complaint of fever, fatigue, non-productive cough and painful rash. Scattered erythematous papules and subcutaneous nodules on exam were diagnosed as folliculitis and treated with topical antibiotics. Considering a normal pulmonary exam and negative COVID-19 and influenza point of care testing, conservative management was recommended for presumed viral rhinitis. She later presented to the emergency department with progressive flu-like symptoms and rash. Imaging showed pulmonary consolidation and subcutaneous soft tissue nodules on her chest and abdomen. She was admitted for treatment of community acquired pneumonia (CAP) and further workup of pustular rash. Empiric antibiotics were administered for CAP while further workup was obtained, which proved unremarkable. Infectious disease was unable to discern an identifiable infectious or autoimmune etiology for her worsening skin nodules. Preliminary wound cultures were unremarkable, and the patient was discharged on oral steroids. The patient subsequently presented to multiple emergency departments and her PCP, receiving additional antibiotics despite worsening symptoms. The patient suffered a seizure and cardiac arrest and was admitted to the intensive care unit. Culture data from prior hospitalization grew Blastomyces dermatitidis. Despite empiric amphotericin B and broad-spectrum antibiotics, the patient expired secondary to her advanced disease after 43 days in the ICU.
Discussion: This case demonstrates the importance of treating the whole patient as outlined in the tenets of Osteopathic Medicine. Treating parts of this patient’s presentation in isolation likely contributed to delayed diagnosis and worse outcomes. Blastomycosis is a systemic pyogranulomatous infection that often mimics other diseases. Acute pulmonary infection is often misdiagnosed as a bacterial or viral and chronic pulmonary infection for malignancy or tuberculosis. Extrapulmonary involvement and multiorgan involvement is through hematogenous spread. Those with advanced disease are often immunosuppressed. Definitive diagnosis is made by culture. Serum and urine antigen detection can also be used. Treatment with antifungal agents such as amphotericin B or itraconazole is standard. Diagnosis by early biopsy of lesion or presumptive diagnosis by direct visualization on wet preparation could have led to earlier diagnosis and treatment for this patient.
