Medical Education
Recurrent Gestational Hydronephrosis Management and Screening Considerations
Friday, March 31, 2023
12:00 PM East Coast USA Time
- HH
Hayley D. Hatherly, DO (she/her/hers)
Flight Surgeon
United States Navy
Hanford, California, United States
Presenting Author(s)
Introduction: Renal Colic/hydronephrosis is a rare urological pregnancy complication, with limited publications. This case provides awareness and adds valuable data to aid in future patient management.
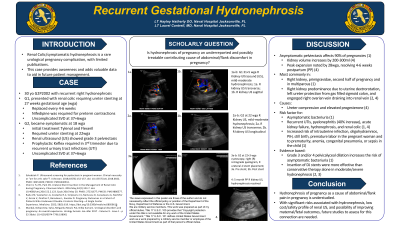
Case Study: 30 yo G2P2002 with recurrent right hydronephrosis.
G1, presented with renal colic and required ureter stenting at 27 weeks gestational age (wga), replaced every 4-6 weeks. Nifedipine was required for preterm contractions, with an uncomplicated SVD at 37+6wga.
G2, became symptomatic at 18 wga, initial treatment Tylenol and Flexeril, but required ureter stenting at 22wga. Renal ultrasound (US) showed grade 3 pelviectasis. Prophylactic Keflex required in 3rd trimester due to recurrent urinary tract infections (UTI). G2 delivered at 37+6wga, uncomplicated SVD.
Discussion: Asymptomatic pyelectasis affects 90% of pregnancies with kidney volume increasing 200-300ml, with serial ultrasounds showing peak expansion by 28wga. Most commonly in the right kidney, primigravidae, second half of pregnancy and in multiparous. Caused in combination by ureter compression and elevated progesterone. Urine retention increases risk of asymptomatic bacteriuria and is a risk factor for recurrent UTIs, pyelonephritis, acute kidney failure, hydronephrosis, and renal colic; this can lead to increased risk of intrauterine infection, oligohydramnios, PIH, still birth, premature labor in the pregnant woman and to prematurity, anemia, congenital pneumonia, or sepsis in the child. Studies found grade 3 and/or 4 pelvicalyceal dilation increased the risk of asymptomatic bacteriuria and insertion of DJ stents were more effective than conservative therapy alone in moderate/severe hydronephrosis.
Hydronephrosis of pregnancy as a cause of abdominal/flank pain in pregnancy is understudied. With significant risks associated with hydronephrosis, low cost/safety profile of renal US, and possibility of improving maternal/fetal outcomes, future studies to assess for this connection are needed.
Case Study: 30 yo G2P2002 with recurrent right hydronephrosis.
G1, presented with renal colic and required ureter stenting at 27 weeks gestational age (wga), replaced every 4-6 weeks. Nifedipine was required for preterm contractions, with an uncomplicated SVD at 37+6wga.
G2, became symptomatic at 18 wga, initial treatment Tylenol and Flexeril, but required ureter stenting at 22wga. Renal ultrasound (US) showed grade 3 pelviectasis. Prophylactic Keflex required in 3rd trimester due to recurrent urinary tract infections (UTI). G2 delivered at 37+6wga, uncomplicated SVD.
Discussion: Asymptomatic pyelectasis affects 90% of pregnancies with kidney volume increasing 200-300ml, with serial ultrasounds showing peak expansion by 28wga. Most commonly in the right kidney, primigravidae, second half of pregnancy and in multiparous. Caused in combination by ureter compression and elevated progesterone. Urine retention increases risk of asymptomatic bacteriuria and is a risk factor for recurrent UTIs, pyelonephritis, acute kidney failure, hydronephrosis, and renal colic; this can lead to increased risk of intrauterine infection, oligohydramnios, PIH, still birth, premature labor in the pregnant woman and to prematurity, anemia, congenital pneumonia, or sepsis in the child. Studies found grade 3 and/or 4 pelvicalyceal dilation increased the risk of asymptomatic bacteriuria and insertion of DJ stents were more effective than conservative therapy alone in moderate/severe hydronephrosis.
Hydronephrosis of pregnancy as a cause of abdominal/flank pain in pregnancy is understudied. With significant risks associated with hydronephrosis, low cost/safety profile of renal US, and possibility of improving maternal/fetal outcomes, future studies to assess for this connection are needed.
