Clinical: General Topics
Pediatric COVID Encephalopathy
Friday, March 31, 2023
12:00 PM East Coast USA Time

Jesse Hunt, OMS (she/her/hers)
Medical Student
Edward Via College of Osteopathic Medicine- Auburn
Box Springs, Georgia, United States
Presenting Author(s)
Introduction: The COVID-19 pandemic, caused by the novel coronavirus SARS-CoV-2, has a great burden on the world due to its high morbidity and mortality. Symptom severities range from completely asymptomatic to severe disease leading to death. Neurological complications due to the virus that have been reported are cerebrovascular disease, Guillain- Barre syndrome, myositis, neuropathies, meningoencephalitis, rhombencephalitis, and acute disseminated encephalomyelitis. One presentation of COVID-19 is encephalopathy, especially common among the severely afflicted patients that are hospitalized. Yet, management for encephalopathy from COVID-19 is still unclear. Cases of COVID encephalopathy have not been well described in children, nor has the management.
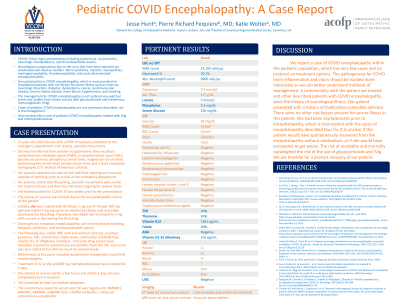
Case Study: In this case report we describe a case of pediatric COVID encephalopathy in a patient with a history of epilepsy that was treated with methylprednisolone and intravenous immunoglobulin (IVIg) with full recovery. The patient presented with irregular, spastic movements that were different than her typical seizures and she was sedated with benzodiazepines and antipsychotics. Several labs were taken to rule out viral and bacterial meningitis, autoimmune encephalitis, and thyroid encephalopathy, including a lumbar puncture with PCR and blood count, complete blood count, comprehensive metabolic panel, computed tomography with and without contrast, magnetic resonance imaging with and without contrast, cerebrospinal fluid cultures, blood cultures, thyroid stimulating hormone levels, vitamin B12 levels, folate levels, antinuclear antibody levels, vitamin D levels, urinalysis, urine drug screen, an autoimmune panel on the serum and cerebrospinal fluid and a rapid COVID test. The only significant finding from these tests was a positive COVID test, although the autoimmune panel was still pending at time of treatment. At this time, we initiated treatment with methylprednisolone and intravenous immunoglobulin (IVIg) because of suspected autoimmune encephalitis or COVID encephalopathy, in which treatments are similar for adult patients. Within 24 hours the patient was returning to her baseline and within five days was completely back to baseline. After discharge, the autoimmune panels for the cerebrospinal fluid and serum had resulted and were both negative.
Discussion: The pathogenesis for COVID brain inflammation and injury should be studied more intensively, so we can better understand methods of management. We need to understand how COVID-19 chemically and structurally impacts the nervous system, with special attention to patients that have underlying nervous system abnormalities, such as this patient with epilepsy. Lastly, we need to define how to treat encephalopathy presumed to be caused by COVID-19, especially in the pediatric population.
Case Study: In this case report we describe a case of pediatric COVID encephalopathy in a patient with a history of epilepsy that was treated with methylprednisolone and intravenous immunoglobulin (IVIg) with full recovery. The patient presented with irregular, spastic movements that were different than her typical seizures and she was sedated with benzodiazepines and antipsychotics. Several labs were taken to rule out viral and bacterial meningitis, autoimmune encephalitis, and thyroid encephalopathy, including a lumbar puncture with PCR and blood count, complete blood count, comprehensive metabolic panel, computed tomography with and without contrast, magnetic resonance imaging with and without contrast, cerebrospinal fluid cultures, blood cultures, thyroid stimulating hormone levels, vitamin B12 levels, folate levels, antinuclear antibody levels, vitamin D levels, urinalysis, urine drug screen, an autoimmune panel on the serum and cerebrospinal fluid and a rapid COVID test. The only significant finding from these tests was a positive COVID test, although the autoimmune panel was still pending at time of treatment. At this time, we initiated treatment with methylprednisolone and intravenous immunoglobulin (IVIg) because of suspected autoimmune encephalitis or COVID encephalopathy, in which treatments are similar for adult patients. Within 24 hours the patient was returning to her baseline and within five days was completely back to baseline. After discharge, the autoimmune panels for the cerebrospinal fluid and serum had resulted and were both negative.
Discussion: The pathogenesis for COVID brain inflammation and injury should be studied more intensively, so we can better understand methods of management. We need to understand how COVID-19 chemically and structurally impacts the nervous system, with special attention to patients that have underlying nervous system abnormalities, such as this patient with epilepsy. Lastly, we need to define how to treat encephalopathy presumed to be caused by COVID-19, especially in the pediatric population.
