Medical Education
Patient Perception of the Semantics of Medical Students: Am I a Medical Student or a Student Doctor?
Friday, March 31, 2023
12:00 PM East Coast USA Time
- BN
Brianna Nghiem, OMS
Rowan-Virtua School of Osteopathic Medicine
Cherry Hill, New Jersey, United States
Presenting Author(s)
Background and Hypothesis: Patients may perceive medical students differently depending on one of two titles that are traditionally used in clinical settings: “medical student” or “student doctor.” Previous studies have indicated that patient understanding of the medical hierarchy is poor and that misunderstanding the role of providers has been found to adversely affect patient safety, trust, and satisfaction. To further understand this relationship, this study investigates differences in patient perception of the terms “medical student” and “student doctor” in university-affiliated and private family practices. It is hypothesized that patients of a university-affiliated family practice will have a greater understanding of a student’s level of training and stronger preferences towards either term due to increased exposure of students.
Methods: An anonymous survey was administered to a convenience sample of patients at five osteopathic family medicine outpatient offices. 259 patients were recruited and completed a paper survey. Inclusion criteria included patients of the family practice who were above 18 years old irrespective of gender. Individuals who were under 18 years old were excluded. Six questions addressed demographic information including sex, age, ethnicity, education level, occupation level, and industry. Seven questions assessed patient perception and preference regarding the titles of “medical student” and “student doctor” in the outpatient setting and hospital setting. Assessment of the differences in patient perceptions was achieved with standard summary statistics and Chi-square analysis.
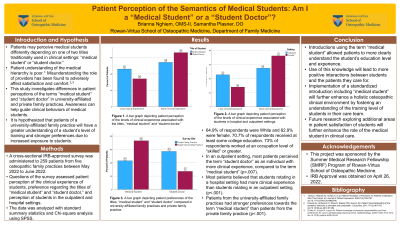
Results: Of the 259 patients who responded to the survey, 64.9% were White and 62.9% were female. 70.7% of respondents received at least some college education. 73% of respondents worked at an occupation level of “skilled” or greater. In an outpatient setting, most patients perceived the term “student doctor” as an individual with more clinical experience, compared to the term “medical student” (p=.007). However, most patients believed that students rotating in a hospital setting had more clinical experience than students rotating in an outpatient setting (p <.001). In addition, patients from a university-affiliated family practice had stronger preferences towards the term “medical student” than patients from a private family practice (p <.001).
Conclusion: Awareness of patient preferences can help guide clinical behaviors of medical students. Introductions using the term “medical student” allowed patients to more clearly understand the student’s education level and experience. Use of this knowledge will lead to more positive interactions between students and the patients they care for. Implementation of a standardized introduction including “medical student” will further enhance a holistic osteopathic clinical environment by fostering an understanding of the training level of students in their care team. Future research exploring additional areas in patient satisfaction of students will enhance the role of medical students in clinical care.
Acknowledgement of Research Study Sponsors and IRB: This project was sponsored by the Summer Medical Research Fellowship (SMRF) Program of Rowan-Virtua School of Osteopathic Medicine. Institutional Review Board (IRB) Approval was obtained on April 26, 2022.
Methods: An anonymous survey was administered to a convenience sample of patients at five osteopathic family medicine outpatient offices. 259 patients were recruited and completed a paper survey. Inclusion criteria included patients of the family practice who were above 18 years old irrespective of gender. Individuals who were under 18 years old were excluded. Six questions addressed demographic information including sex, age, ethnicity, education level, occupation level, and industry. Seven questions assessed patient perception and preference regarding the titles of “medical student” and “student doctor” in the outpatient setting and hospital setting. Assessment of the differences in patient perceptions was achieved with standard summary statistics and Chi-square analysis.
Results: Of the 259 patients who responded to the survey, 64.9% were White and 62.9% were female. 70.7% of respondents received at least some college education. 73% of respondents worked at an occupation level of “skilled” or greater. In an outpatient setting, most patients perceived the term “student doctor” as an individual with more clinical experience, compared to the term “medical student” (p=.007). However, most patients believed that students rotating in a hospital setting had more clinical experience than students rotating in an outpatient setting (p <.001). In addition, patients from a university-affiliated family practice had stronger preferences towards the term “medical student” than patients from a private family practice (p <.001).
Conclusion: Awareness of patient preferences can help guide clinical behaviors of medical students. Introductions using the term “medical student” allowed patients to more clearly understand the student’s education level and experience. Use of this knowledge will lead to more positive interactions between students and the patients they care for. Implementation of a standardized introduction including “medical student” will further enhance a holistic osteopathic clinical environment by fostering an understanding of the training level of students in their care team. Future research exploring additional areas in patient satisfaction of students will enhance the role of medical students in clinical care.
Acknowledgement of Research Study Sponsors and IRB: This project was sponsored by the Summer Medical Research Fellowship (SMRF) Program of Rowan-Virtua School of Osteopathic Medicine. Institutional Review Board (IRB) Approval was obtained on April 26, 2022.
