Medical Education
PAINFUL EPIDIDYMAL MASS TURNED OUT TO BE THE RARE EPIDIDYMAL LEIOMYOSARCOMA
Friday, March 31, 2023
12:00 PM East Coast USA Time
- KL
Kelly Le, DO (she/her/hers)
Naval Hospital Jacksonville
Jacksonville, Florida, United States
Presenting Author(s)
Introduction: Epididymal leiomyosarcoma (LMS) is a rare disease with high recurrence which can easily be misdiagnosed [4]. LMS is accounting for 1-2% of genitourinary malignancies, only 2% of those are epididymal LMS [1]. Like most genitourinary malignancies, epididymal LMS typically presents as painless and slow growing mass. However, we encountered a case of epididymal LMS as a painful mass that could have been missed without further evaluation.
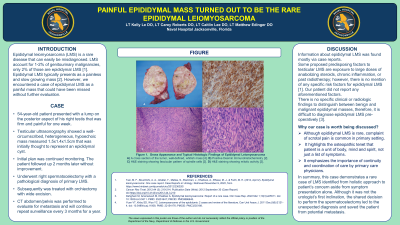
Case Study: 54-year-old patient presented with a lump on the posterior aspect of his right testicle that was firm and painful for one week. Testicular ultrasonography showed a well-circumscribed, heterogeneous, hypoechoic mass measured 1.5x1.4x1.5cm that was initially thought to represent an epididymal cyst with plan of continued monitoring. The patient followed up 2 months later without improvement. He underwent right spermatocelectomy with a pathological diagnosis of primary LMS. Subsequently, he was treated with orchiectomy with wide excision. CT abdomen/pelvis was performed to evaluate for metastasis and will continue repeat surveillance every 3 months for a year.
Discussion: Information about epididymal LMS was found mostly via case reports. Some proposed predisposing factors to testicular LMS are exposure to large doses of anabolizing steroids, chronic inflammation, or past radiotherapy; however, there is no mention of any specific risk factors for epididymal LMS [1]. Our patient did not report any aforementioned factors. In addition, since there are no specific clinical or radiologic findings to distinguish between benign and malignant epididymal masses, it is difficult to diagnose epididymal LMS pre-operatively [2].
Our case is worth being discussed not only due to its rare prevalence and infrequent occurrence in primary care setting, but it also highlights the osteopathic tenet that patient is a unit of body, mind and spirit, not just a list of symptoms. Since most paratesticular masses are benign [3], this patient’s uncommon diagnosis would not have been discovered if his family physician did not schedule serial clinical follow up visits with him or perform meticulous coordination of care with the urologist. This case demonstrates a rare case of LMS identified from holistic approach to patient’s concern aside from symptom presentation alone. Although it was not the urologist’s first inclination, the shared decision to perform the spermatocelectomy led to the unexpected diagnosis and saved the patient from potential metastasis or even his life.
Case Study: 54-year-old patient presented with a lump on the posterior aspect of his right testicle that was firm and painful for one week. Testicular ultrasonography showed a well-circumscribed, heterogeneous, hypoechoic mass measured 1.5x1.4x1.5cm that was initially thought to represent an epididymal cyst with plan of continued monitoring. The patient followed up 2 months later without improvement. He underwent right spermatocelectomy with a pathological diagnosis of primary LMS. Subsequently, he was treated with orchiectomy with wide excision. CT abdomen/pelvis was performed to evaluate for metastasis and will continue repeat surveillance every 3 months for a year.
Discussion: Information about epididymal LMS was found mostly via case reports. Some proposed predisposing factors to testicular LMS are exposure to large doses of anabolizing steroids, chronic inflammation, or past radiotherapy; however, there is no mention of any specific risk factors for epididymal LMS [1]. Our patient did not report any aforementioned factors. In addition, since there are no specific clinical or radiologic findings to distinguish between benign and malignant epididymal masses, it is difficult to diagnose epididymal LMS pre-operatively [2].
Our case is worth being discussed not only due to its rare prevalence and infrequent occurrence in primary care setting, but it also highlights the osteopathic tenet that patient is a unit of body, mind and spirit, not just a list of symptoms. Since most paratesticular masses are benign [3], this patient’s uncommon diagnosis would not have been discovered if his family physician did not schedule serial clinical follow up visits with him or perform meticulous coordination of care with the urologist. This case demonstrates a rare case of LMS identified from holistic approach to patient’s concern aside from symptom presentation alone. Although it was not the urologist’s first inclination, the shared decision to perform the spermatocelectomy led to the unexpected diagnosis and saved the patient from potential metastasis or even his life.
