Medical Education
Assessing Attitudes of Homelessness using Street Medicine Curriculum in Family Medicine Residency
Friday, March 31, 2023
12:00 PM East Coast USA Time

Jaclyn E. Sylvain, DO (she/her/hers)
Family Practice Resident
Munson Medical Center
Traverse City, Michigan, United States
Presenting Author(s)
Background and Hypothesis: Street Medicine is a burgeoning field of medicine aimed at delivering healthcare directly to people experiencing homelessness where they live. While street medicine programs at residency training and medical schools have become more commonplace, a formal curriculum and utilization of a validated survey tool on its impact is lacking. Using a validated survey tool, the Health Professional Attitudes Towards the Homeless Inventory (HPATHI), this study aimed to assess the attitudes and confidence levels of residency faculty, residents and medical students before and after a two-hour educational session on homelessness and street medicine.
Methods: The study population consisted of members of the Munson Family Practice residency program, including medical residents, faculty and medical students from MSUCOM based at Munson Medical Center, attending the Street Medicine educational session on 9/22/22 and 9/29/22 The two-hour educational session included a live lecture by Dr. Klee, video recorded lecture by Dr. Sylvain and video clips from Street Medicine Institute. The lecture content included statistical data about the national problem of homelessness, review of risk factors to becoming homeless and discussion of the medical problems that are both caused by or worsened by being homeless. Exclusion criteria included residents, medical students and faculty who chose not to participate in survey or were not present for didactic lecture. Out of a possible 22 participants, one individual met the exclusion criteria. A pre/post study design was utilized with anonymous, self-administered 21-question online HPATHI surveys emailed to participants before and after participation in the Street Medicine educational session. Each survey item was assessed using a 5-point Likert scale ranging from “Strongly Disagree = 0” to “Strongly Agree =5" and descriptive statistics were examined for survey measures pre- and post-curriculum lecture.
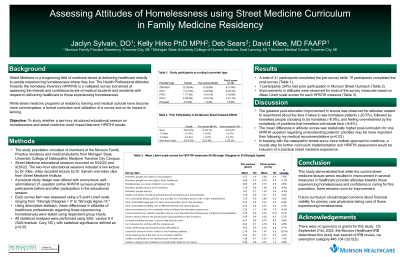
Results: A total of 21 participants completed the survey before the Street Medicine educational session, while 19 participants completed the survey after the educational session. Improvements in attitudes were observed for most of the survey measures based on Mean Likert scale scores for each HPATHI measure. The greatest post-education improvement in Mean Likert scale scores was observed for attitudes related to resentment about the time it takes to see homeless patients (-20.5%), followed by homeless people choosing to be homeless (-8.9%), and feeling overwhelmed by the complexity of problems that homeless individuals face (-8.8%). The mean difference in attitude scores were statistically higher post-curriculum with regard to one HPATHI question regarding understanding patients’ priorities may be more important than following my medical recommendations (p=0.03).
Conclusion: This study has shown that while the current street medicine lecture series resulted in improvement in several measures in healthcare provider attitudes towards those experiencing homelessness and confidence in caring for this population, there is room for improvement. In keeping with the osteopathic tenets and a more holistic approach to medicine, a crucial step for further curriculum implementation and HPATHI assessment would be inclusion of a practical street medicine experience in combination with didactic material.
Acknowledgement of Research Study Sponsors and IRB: On September 21st, 2022, the Munson Healthcare IRB determined this study was exempt of IRB review, via exemption category #46.104 (d)(1)(2i).
Methods: The study population consisted of members of the Munson Family Practice residency program, including medical residents, faculty and medical students from MSUCOM based at Munson Medical Center, attending the Street Medicine educational session on 9/22/22 and 9/29/22 The two-hour educational session included a live lecture by Dr. Klee, video recorded lecture by Dr. Sylvain and video clips from Street Medicine Institute. The lecture content included statistical data about the national problem of homelessness, review of risk factors to becoming homeless and discussion of the medical problems that are both caused by or worsened by being homeless. Exclusion criteria included residents, medical students and faculty who chose not to participate in survey or were not present for didactic lecture. Out of a possible 22 participants, one individual met the exclusion criteria. A pre/post study design was utilized with anonymous, self-administered 21-question online HPATHI surveys emailed to participants before and after participation in the Street Medicine educational session. Each survey item was assessed using a 5-point Likert scale ranging from “Strongly Disagree = 0” to “Strongly Agree =5" and descriptive statistics were examined for survey measures pre- and post-curriculum lecture.
Results: A total of 21 participants completed the survey before the Street Medicine educational session, while 19 participants completed the survey after the educational session. Improvements in attitudes were observed for most of the survey measures based on Mean Likert scale scores for each HPATHI measure. The greatest post-education improvement in Mean Likert scale scores was observed for attitudes related to resentment about the time it takes to see homeless patients (-20.5%), followed by homeless people choosing to be homeless (-8.9%), and feeling overwhelmed by the complexity of problems that homeless individuals face (-8.8%). The mean difference in attitude scores were statistically higher post-curriculum with regard to one HPATHI question regarding understanding patients’ priorities may be more important than following my medical recommendations (p=0.03).
Conclusion: This study has shown that while the current street medicine lecture series resulted in improvement in several measures in healthcare provider attitudes towards those experiencing homelessness and confidence in caring for this population, there is room for improvement. In keeping with the osteopathic tenets and a more holistic approach to medicine, a crucial step for further curriculum implementation and HPATHI assessment would be inclusion of a practical street medicine experience in combination with didactic material.
Acknowledgement of Research Study Sponsors and IRB: On September 21st, 2022, the Munson Healthcare IRB determined this study was exempt of IRB review, via exemption category #46.104 (d)(1)(2i).
