Medical Education
Adherence to National Insulin Guidelines at the Hinsdale Family Medicine Clinic
Friday, March 31, 2023
12:00 PM East Coast USA Time
- AC
Poster Presenter(s)
Background and Hypothesis: Uncontrolled T2 diabetics often face long term serious complications of hyperglycemia including neuropathy, nephropathy and retinopathy. Many patients with T2DM who would benefit from insulin therapy are reluctant to be started on insulin therapy. Physician knowledge and comfort with insulin management in the uncontrolled T2DM population is an important factor that can serve to help bridge gaps in patient care and positively influence long term preventive outcomes in T2DM patients.
We aim to understand and identify reasons for physician non-adherence in insulin initiation within our clinic's diabetic patient population for the purpose of identifying systemic gaps that can be improved upon for our diabetic patients.
Methods: This will be a survey study with the specific aim and goal of identifying provider knowledge gaps or provider hesitancy with initiating and managing insulin in a subset of T2DM clinic patients who meet insulin criteria but are not on insulin. Patient data and provider input will be obtained from the Hinsdale Family Medicine Clinic (HFMC) and residency. Identified knowledge gaps or discomfort with insulin initiation and management was addressed with educational conferences and resources. The goal is to identify provider gaps to improve long-term patient outcomes for our clinic’s subset of T2DM patients who meet insulin criteria.
Of the 35 possible providers onsite between attending physicians and resident physicians, 7 provided surveyed responses for the study. There were 215 identified diabetic patients at HFMC between 2020-2022, of which 83 met criteria for uncontrolled T2DM and guidelines for starting insulin (A1c>9).
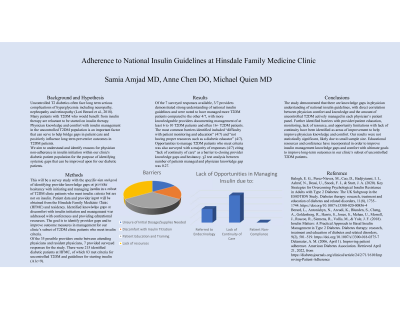
Results: Of the 7 surveyed responses available, 3/7 providers demonstrated strong understanding of national insulin guidelines and were noted to have managed more T2DM patients compared to the other 4/7, with more knowledgeable providers documenting management of at least 6 to 10 T2DM patients and often 16+ T2DM patients. The most common barriers identified included “difficulty with patient monitoring and education” (4/7) and “not having proper resources such as a diabetic educator” (4/7). Lack of opportunities to manage T2DM patients who meet criteria was also surveyed, with a majority of responses (4/7) citing “lack of continuity of care” as a barrier to provider knowledge and comfort. χ2 test analysis between number of patients managed and physician knowledge gap was 0.27.
Conclusion: The study demonstrated that there are knowledge gaps in physician understanding of national insulin guidelines, with direct correlation between physician comfort/knowledge and the amount of uncontrolled T2DM actively managed in each physician’s HFMC patient panel. Further identified barriers with provider/patient education, monitoring, lack of resources, and lack of continuity are areas to be improved upon in order to address knowledge gap or comfort level. Our results were not statistically significant, likely due to small sample size. Going forward, we aim to use the results of this study to implement educational resources and conferences to bridge the physician knowledge/comfort gap and ultimately improve long-term outcomes for our clinic’s subset of uncontrolled T2DM patients.
Acknowledgement of Research Study Sponsors and IRB: There are no study sponsors nor grants received for the study. This study was deemed IRB exempt and is a QI project.
We aim to understand and identify reasons for physician non-adherence in insulin initiation within our clinic's diabetic patient population for the purpose of identifying systemic gaps that can be improved upon for our diabetic patients.
Methods: This will be a survey study with the specific aim and goal of identifying provider knowledge gaps or provider hesitancy with initiating and managing insulin in a subset of T2DM clinic patients who meet insulin criteria but are not on insulin. Patient data and provider input will be obtained from the Hinsdale Family Medicine Clinic (HFMC) and residency. Identified knowledge gaps or discomfort with insulin initiation and management was addressed with educational conferences and resources. The goal is to identify provider gaps to improve long-term patient outcomes for our clinic’s subset of T2DM patients who meet insulin criteria.
Of the 35 possible providers onsite between attending physicians and resident physicians, 7 provided surveyed responses for the study. There were 215 identified diabetic patients at HFMC between 2020-2022, of which 83 met criteria for uncontrolled T2DM and guidelines for starting insulin (A1c>9).
Results: Of the 7 surveyed responses available, 3/7 providers demonstrated strong understanding of national insulin guidelines and were noted to have managed more T2DM patients compared to the other 4/7, with more knowledgeable providers documenting management of at least 6 to 10 T2DM patients and often 16+ T2DM patients. The most common barriers identified included “difficulty with patient monitoring and education” (4/7) and “not having proper resources such as a diabetic educator” (4/7). Lack of opportunities to manage T2DM patients who meet criteria was also surveyed, with a majority of responses (4/7) citing “lack of continuity of care” as a barrier to provider knowledge and comfort. χ2 test analysis between number of patients managed and physician knowledge gap was 0.27.
Conclusion: The study demonstrated that there are knowledge gaps in physician understanding of national insulin guidelines, with direct correlation between physician comfort/knowledge and the amount of uncontrolled T2DM actively managed in each physician’s HFMC patient panel. Further identified barriers with provider/patient education, monitoring, lack of resources, and lack of continuity are areas to be improved upon in order to address knowledge gap or comfort level. Our results were not statistically significant, likely due to small sample size. Going forward, we aim to use the results of this study to implement educational resources and conferences to bridge the physician knowledge/comfort gap and ultimately improve long-term outcomes for our clinic’s subset of uncontrolled T2DM patients.
Acknowledgement of Research Study Sponsors and IRB: There are no study sponsors nor grants received for the study. This study was deemed IRB exempt and is a QI project.
